Stable, Aesthetic and Healthy – Dr Carlo Brogna
Featured Products Promotional FeaturesPosted by: Dental Design 5th March 2019

Dr Carlo Brogna is a highly experienced dentist from Italy. Here, he shares an interesting recent case that demonstrates the importance of soft and hard tissue stability for long-term success of a dental implant.

Patient presentation
This 30-year-old female patient initially presented to the practice a few years ago, as she required a partial restoration of her upper right arch. She was missing the UR4, UR5 and UR6, with a dental implant already placed in the UR5 position by another dentist (Figure 1). This had been in situ since 2012.
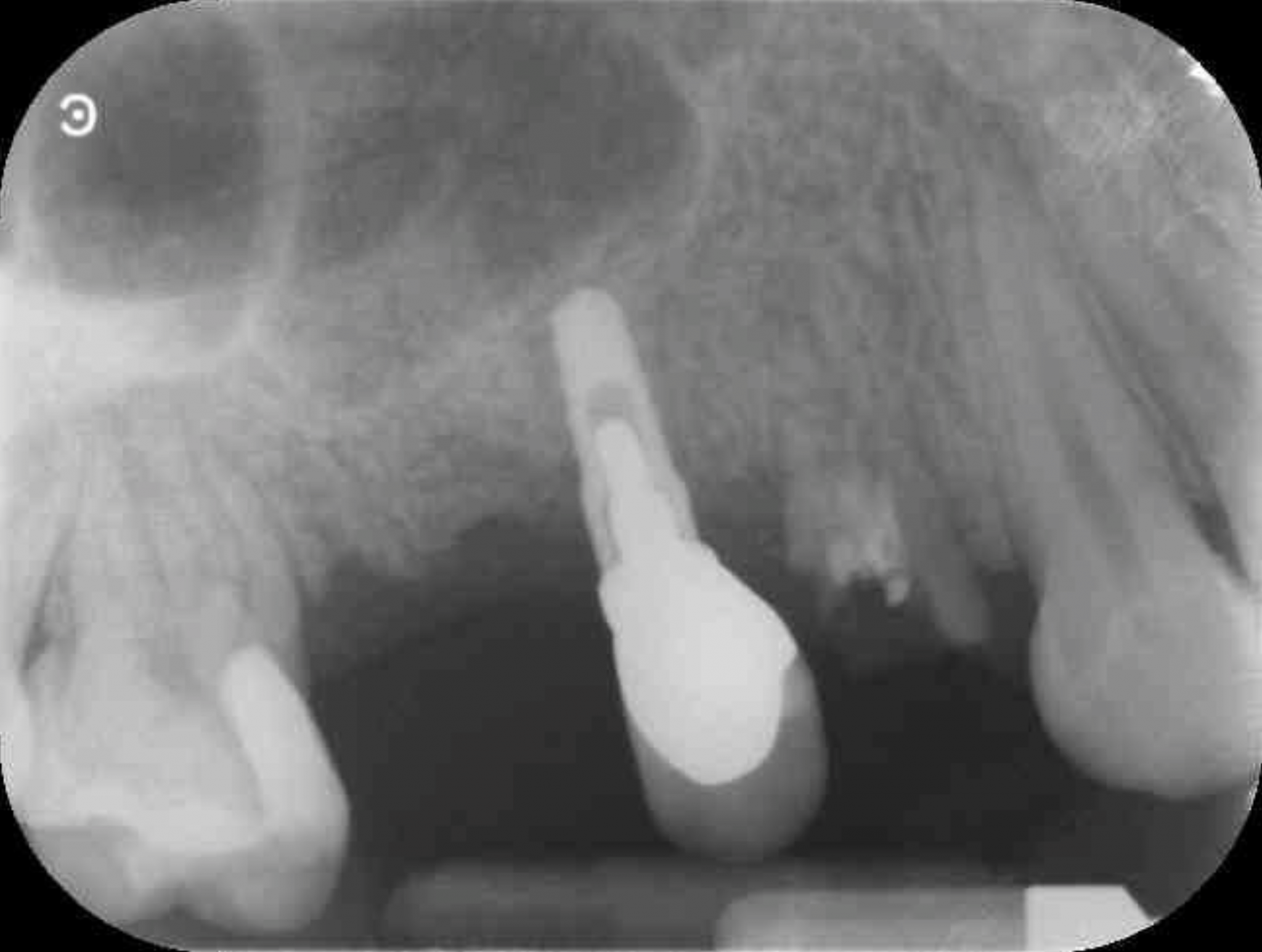
Fig: 1
Treatment
In order to replace the missing teeth either side of the existing implant, the possible treatment options included a bridge or two new implants. The latter was the preferred choice of the patient.
As such, two dental implants from TBR were placed following a standard placement protocol. A Z1 tissue level implant with a zirconia collar was placed in the position of the UR4 in 2015, which was chosen in order to maximise the aesthetic outcome of surgery. Later on in 2016, a bone level titanium TBR implant was placed at the UR6 (Figures 2 and 3). As the patient’s smile line did not expose the UR6, there were no aesthetic concerns for this implant and so the bone level implant was chosen.
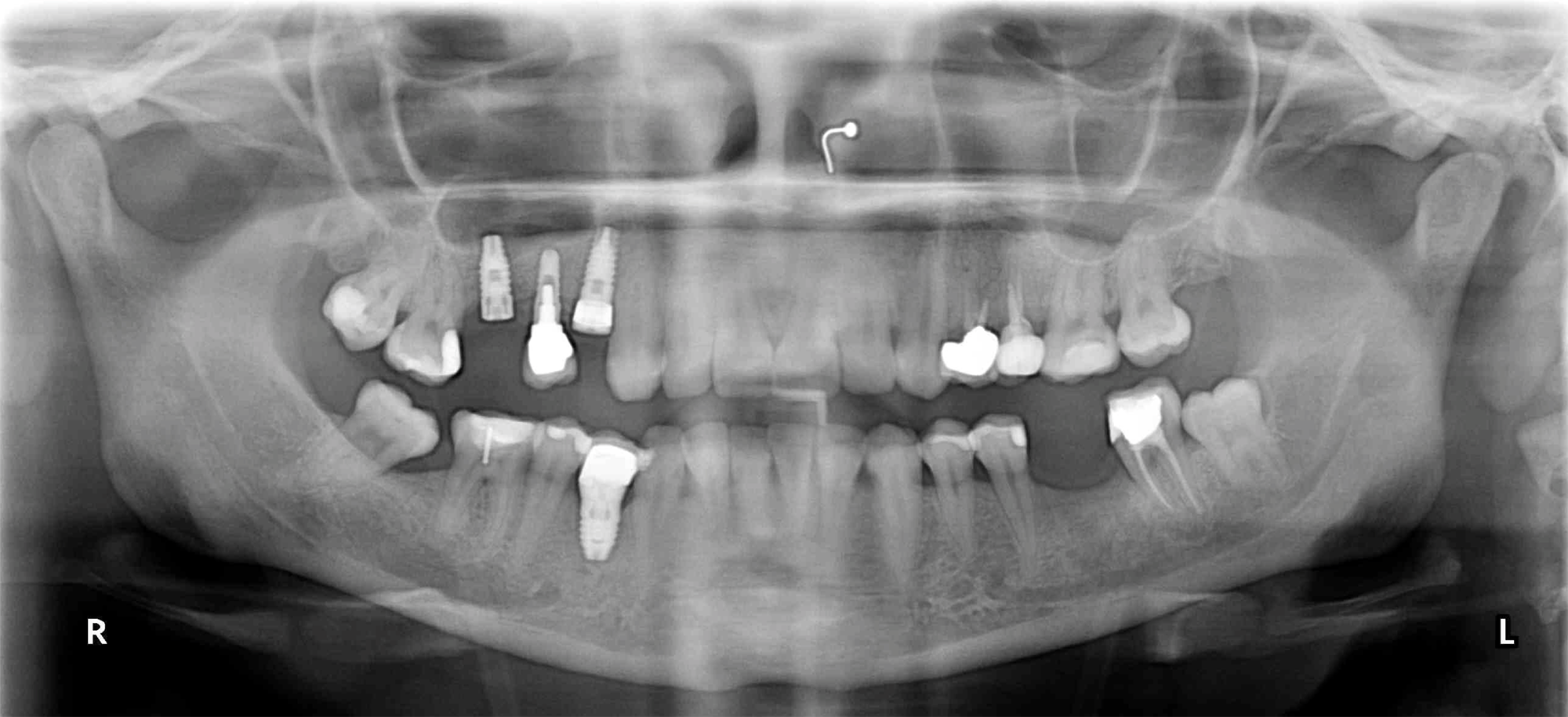
Fig: 2
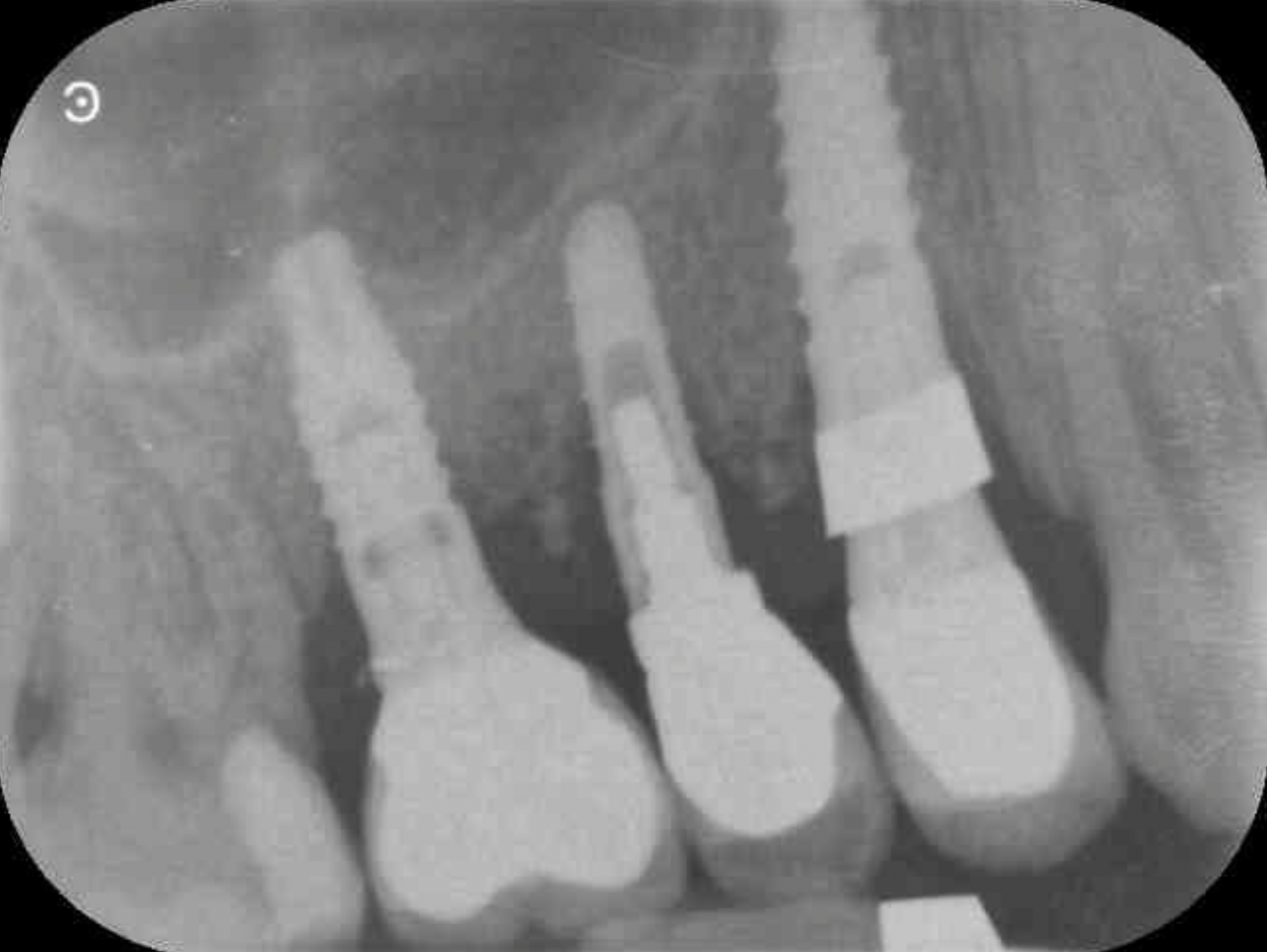
Fig: 3
Both the implants were restored with cement-retained, metal-fused-to-ceramic restorations during their respective restoration phases. The ideal restorative material for both implants in this case would have been zirconia, but due to the patient’s financial restrictions, we had to deliver treatment that was more economical for her. Despite this, the reduction in bacterial proliferation by the zirconia collar meant that the metal-ceramic restoration was still very compatible.
This case was particularly interesting to monitor as it involved three different adjacent implants from two different manufacturers. It was remarkable to see the difference in soft tissue response between the various implants.
Screw vs cement retention
A note should also be made here with regards to the cementation of the restorations. There is a growing trend among clinicians around the globe to favour screw-retained restorations over cement-retained alternatives. I believe this is often due to the fact that most manufacturers fabricate bone level titanium implants – excess cement during the restorative phase of treatment can cause peri-implantitis or various other post implant complications. Even though screw-retained restorations are less aesthetic, this is why they are commonly chosen over cement-retained alternatives.
A key benefit of the Z1 implant is that the zirconia collar is in contact with the gingiva, creating attachment and preventing cement infiltration, as well as any consequential complications. Another advantage is that the Z1 implant provides freedom for the clinician to choose between screw- and cement-retained restoration, according to each individual case. It supports an analogue or CAD/CAM workflow for both.
Clinical development
In early 2018, the patient returned for a standard review appointment. Unfortunately, the oldest dental implant had become very mobile and was failing completely (Figure 4). Significant bone loss could be identified from the radiographs around the UR5 (Figure 5) and this had lead to an aesthetic defect that the patient was not happy with.
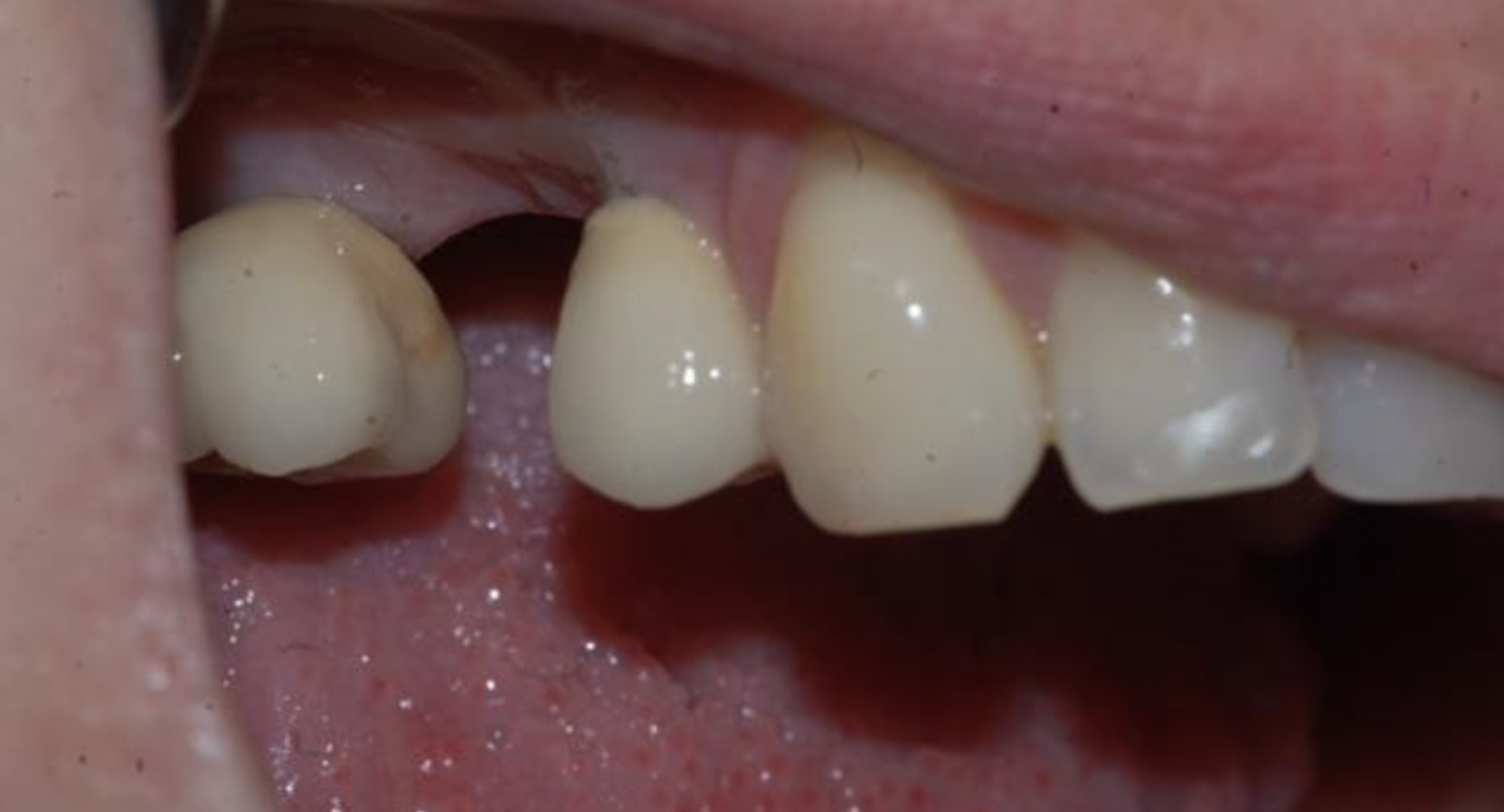
Fig:4
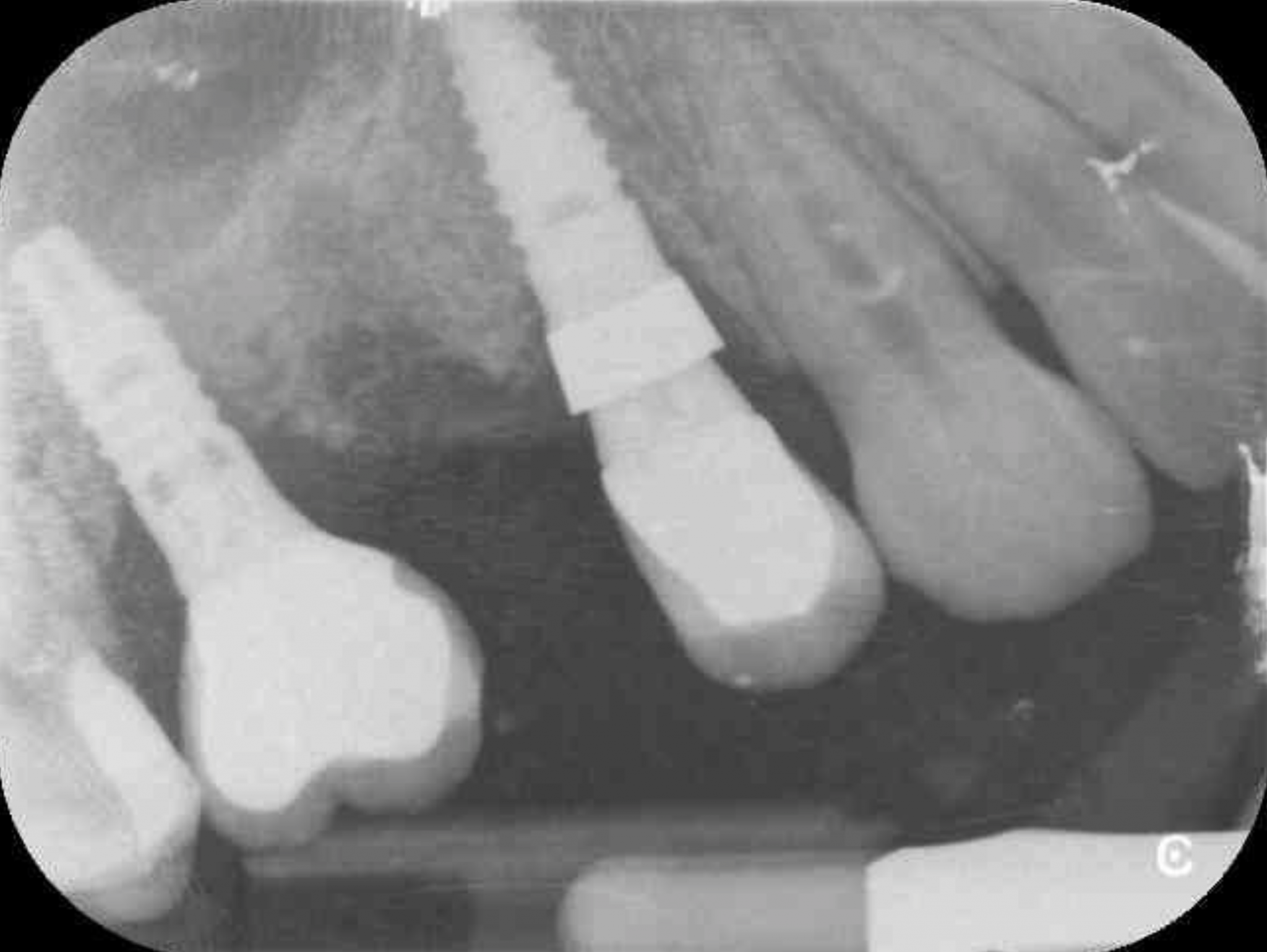
Fig: 5
Proven stability
Impressively, the two TBR implants placed most recently hadn’t suffered from bone loss, despite the defect that had developed around the middle failing implant. The two TBR implants continued to exhibit good stability and more than acceptable aesthetics, particularly the Z1 implant with the zirconia collar. This demonstrated how the zirconia collar created creeping attachment of the gingiva, preventing the loss of either soft tissue or bone. This is fundamental for both clinician and patient, as it provides a guarantee of long-term success of the function and aesthetics of the dental implant. The zirconia collar effectively acts as a protective shield around the implant, significantly reducing the potential for bacteria to infiltrate and colonise the soft tissue. In this way, it encourages stability of the gingiva and decreases the potential risk of peri-implant complications developing in the future.
Looking ahead
For this particular case, we are planning to place another Z1 implant with zirconia collar in the UR5 position. This will likely require bone regeneration therapy in order to replace the loss of bone and facilitate successful osseointegration of the new implant.
I would also be interested in utilising the Z1 implant for CAD/CAM full arch reconstructions with guided surgery protocols. The tools are already available to allow this, so my next step as a clinician will be to look into it and make use of the benefits afford by the Z1 in more cases.
For more information on the Z1 implant, visit tbr.dental, email support@denkauk.comor call 0800 707 6212
Author bio:
Dr. Carlo Brogna has worked in a private practice in Italy since 2004. He has completed degrees in Dentistry and Prosthodontics, has an MSc in Orthodontics, Gnathology and Orofacial Pain, and an MSc in Medicine and Surgery. He has lectured and published extensively on the topic of a multidisciplinary aesthetic approach, combining implantology and orthodontics.
No Comments
No comments yet.
Sorry, the comment form is closed at this time.



