The damaging effects of acid exposure – Flo Couper – Calcivis
Featured Products Promotional FeaturesPosted by: Dental Design 12th December 2019

 The damaging effects of acid exposure
The damaging effects of acid exposure
It has been reported that as many as 77 per cent of adults have some form of tooth wear and levels of moderate tooth wear have also increased, especially in young adults.[1] As dental professionals are aware, tooth wear is a natural part of ageing but pathological tooth wear often involves an erosive component, such as acid.
Dental erosion is defined as the irreversible loss of dental hard tissue by a
chemical process not involving bacteria, [2] which is what differentiates it from caries.
Prolonged exposure from acids on the tooth surface can result in the rapid or excessive dissolution of surface minerals layer by layer and the development of lesions that are susceptible to continued erosion and abrasion.[3] It is a progressive condition that may occur gradually but it has the potential to cause significant damage to the structure of the teeth along with functional, aesthetic and sensitivity problems. The clinical features of dental erosion include: increased loss of enamel surface, facets or wear on the teeth or restorations, incisal translucency, chipping, cupping out of occlusal surfaces and the exposure of the dentine. [4]
Acids that can cause dental erosion can originate from intrinsic, extrinsic and to a lesser extent, environmental sources.[5] For instance, dental erosion due to intrinsic factors is usually caused by gastric acid entering the oral cavity during vomiting episodes or persistent gastro-oesophageal reflux over a long period of time. This can occur as a side effect of certain underlying conditions or medications, as well as alcohol or drug abuse, morning sickness during pregnancy and certain psychosomatic disorders such as extreme stress or anorexia and bulimia nervosa.[6] Extrinsic acids are largely dietary acids such as citric acid, phosphoric acid, ascorbic acid, malic acid, tartaric acid and carbonic acids, which are present in a variety of products such as fruits and juices, soft drinks (still and carbonated), dry wines, pickles and vinegar-containing foods as well as some herbal teas.[7] Environmental sources are usually due to exposure to acidic fumes. Certainly, workers in factories without proper safeguards as well as swimming pools with low pH due to inadequate maintenance, have been implicated.[8]
As well as acids, any factor or condition that results in a low salivary flow rate increases the risk of dental erosion due to reduced pH buffering capacity. To explain: in order to maintain a healthy oral environment, the normal salivary pH needs to be within the 6 to 7 range. However, in the presence of acids this can reach the critical level of around 5.5pH when calcium and other mineral ions are driven from the enamel resulting in demineralisation.[9] Following an ‘acid attack’, the buffering and protective effects of saliva spring into action and natural recovery usually takes place within 30 to 60 minutes. This entails saliva, which dilutes and neutralises acids to regulate pH levels and transports mineral ions back to the enamel in a process known as remineralisation.
Patients should be made aware that any medications that reduce saliva flow or decrease its pH, can weaken its overall buffering effects against both intrinsic and extrinsic acids.[10] Furthermore, the frequency at which dietary acids are consumed and the time of toothbrushing can increase the risks of dental erosion. For example, if a patient continually snacks or sips juice throughout the day, they are exposing their teeth to repeated attacks from acids without allowing enough time for the enamel to remineralise or repair. Also, some patients may think that brushing the teeth immediately after consuming food will help, but brushing immediately after demineralisation when the tooth enamel is soft, results in the increased loss of dentin surfaces.[11] Rinsing with water or chewing sugar free gum to increase saliva flow is a better strategy but in order to protect the teeth, studies indicate that 30 minutes should elapse before toothbrushing following an erosive acid attack.11
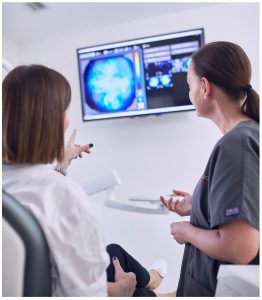
It is the role of dental professionals to educate patients and make them aware of the harmful effects that acids can have on the teeth. They can also support patients in the management of risk factors and making behavioural and dietary changes to prevent further erosive destruction. One of the most effective ways of helping patients to fully understand is to incorporate the CALCIVIS® imaging system into routine examination processes. This innovative device uses bioluminescence to capture images of actively demineralising tooth surfaces, so that practitioners and patients can actually see the effects that acids are having on the teeth. The advantage of the CALCIVIS imaging system is that it is able to detect free calcium ions as they are released from the tooth surfaces at the very early stages, which means that problems can be picked up and addressed before they have a chance to progress or cause irreparable damage. The CALCIVIS imaging system also provides patients with personal information, which both engages and motivates them into making the changes they need to protect their teeth from further damage as well as the need for complex or more invasive treatment in the future.
For more information visit www.CALCIVIS.com
or call 0131 658 5152
References
[1] Public Health England. Delivering better oral health: an evidence-based toolkit for prevention. https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/605266/Delivering_better_oral_health.pdf[Accessed 9th July 2019]
[2] The British Society for Restorative Dentistry. Tooth wear guidelines. https://www.bsrd.org.uk/guidelines/BSRD-Tooth-Wear-Guidelines-KH1-3.pdf [Accessed 9th July 2019]
3 Ravi R.K et al. Non carious lesions due to tooth surface loss: a review. Denal Era – A Journal of Dentistry July-Sept 2003 3(3) 35-38. https://www.researchgate.net/publication/259018999_Non-carious_lesions_due_to_tooth_surface_loss_A_Review
[4] Paryag A et al. Dental erosion and medical conditions. An overview of aetiology, diagnosis and management. West Indian Med J. 2014 Sep; 63(5): 499–502. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4655683/ [Accessed 9th July 2019]
[5] Shaw L et al. Dental erosion – the problem and some practical solutions. British Dental Journal. 1998 186(3) 115-118.http://www.oocities.org/scientistconrad/Colgate_Erosion/Manuscripts/Dental_erosion__the_problem_and_some_practical_solutions.pdf[Accessed 9th July 2019]
[6] Scheutzel P. Etiology of dental erosion – intrinsic factors. Eur J Oral Sci. 1996 Apr;104(2 ( Pt 2)):178-90.https://www.ncbi.nlm.nih.gov/pubmed/8804885 [Accessed 9th July 2019]
[7] Moynihan P et al. Diet, nutrition and the prevention of oral diseases. 2004 Public Health Nutrition: 7(1A), 201–226. https://www.ncbi.nlm.nih.gov/pubmed/14972061 [Accessed 4th April 2018]
[8] Zero DT. Etiology of dental erosion – extrinsic factors. Eur J Oral Sci. 1996 Apr ;104(2 (Pt 2)):162-77. https://www.ncbi.nlm.nih.gov/pubmed/8804884 [Accessed 9th July 2019]
[9] Hemagaran G. et al. Reminalisation of the tooth structure – The future of dentistry. Int. J PharmTech Research. 2014. 6 (2) 487-493. http://sphinxsai.com/2014/PTVOL6/PT=11(487-493)AJ14.pdf
[Accessed 9th July 2019]
[10] Abou Neel E.A, et al. Demineralization–remineralization dynamics in teeth and bone. Int J Nanomedicine. 2016; 11: 4743–4763.https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5034904/ [Accessed 9th July 2019]
[11] Attin T, et al. Brushing abrasion of softened and remineralised dentin: an in-situ study. Caries Res. 2004 Jan-Feb;38(1):62-6. https://www.ncbi.nlm.nih.gov/pubmed/14684979 [Accessed 9th July 2019]
No Comments
No comments yet.
Sorry, the comment form is closed at this time.



