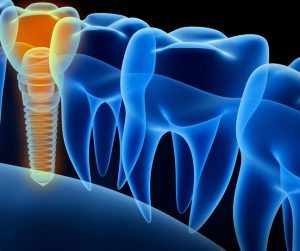
Dental implants are becoming more commonly provided as demand for them continuously rises. With their ability to restore a patient’s smile and confidence, they offer a reliable and aesthetically pleasing solution to missing teeth.
However, despite the advancements in both the surgical and aesthetic aspects of implantology, the preparations and procedures themselves are not of sole involvement. The reality stands that all the hard work and financial input into a new smile is only worthwhile dependent on how the patient cares for their implants – decisively impacting their longevity.
Clinical challenges
Peri-implant disease presents as peri-implantitis and peri-implant mucositis (PIM), and is prevalent as a greatly recognised clinical challenge.[i] With the implant population growing, so too must the preventative methods for better long-term outcomes. For dental professionals, the duty remains in promoting these precautionary measures through effective plaque control – particularly in the interdental regions.
In a recent long-term study, the prevalence of PIM in patients was nearly 46% over 20+ years and approximately 40% of implants showed signs of PIM respectively.[ii] Such evidence highlights that regardless of surgical success and clinical advice, the maintenance of implants is a great source of issues in their longevity.
Interdental importance
Implants, unlike natural teeth, lack the vital periodontal ligament fibres that reduce the bacterial vulnerability of soft-tissue. Once this level of inflammation has begun, it becomes difficult to salvage bone, which reduces in volume at a rapid rate – something extremely difficult to cease.
With the natural dentition, the consequences of interdental neglect can present as gingivitis or caries. However, failure to maintain oral health with implants results in much greater ramifications: the supporting structures make them more susceptible to inflammation, subsequently accelerating peri-implant bone loss, compromising aesthetics and mobility, eventually risking catastrophic implant failure, making interdental cleaning integral.
Research consistently demonstrates the importance of interdental and submucosal care.[iii] Whereas brushing is great for removing the surface-level bacteria, the deeper, harder-to-reach areas more commonly retain plaque leading to subsequent complications. The prosthetic design of implants involves different spatial positioning,[iv] abutments, and connector elements that can create challenging intricacies compared to regular tooth cleaning.[v] This means that even the most thorough and regular toothbrushing can be unsuccessful in removing all harmful plaque.

The flossing compliance problem
Despite the continuous guidance patients are offered, very few adhere to such. A recent study evidences that only 30% of patients use dental floss.[vi] Common reasons for such include the inconvenience and lack of time, as well as sheer discomfort.[vii]
These justifications are only augmented living with implants: dexterity challenges are heightened in weaving floss around fixed prostheses, and overarching access difficulties are caused by the inhibiting geometries of prosthetic contours and connectors.[viii] Furthermore, when patients don’t physically see or feel the damage to their implants immediately, they are less likely to continue such habit.
For clinicians, this presents an ongoing compliance challenge. Beyond the implant itself, peri-implant inflammation is directly linked to systemic inflammation, contributing to further health repercussions.
Dental professionals in prevention
Recommending supportive oral hygiene advice comes in many different forms with interdental flossing being a great choice.[ix] Recent studies indicate that water flossing evidence a fast and simple solution to the removal of dental plaque and reducing gingivitis too. For patients with implants, water flossers can offer ease of access around the prostheses and gentle irrigation of the peri-implant sulcus.[x]
Many find water flossers offer faster and more comfortable than manual options, which assists in the long-term maintenance of such habits – ensuring the preserved health of patients’ implants.
The Ultra Professional Advantage
Certain devices have entered the market, yet the gold standard remains as the Ultra Professional water flosser from WaterpikTM, remaining the most powerful and advanced flosser in the range. With 10 pressure settings, 2 flossing modes, and 5 flossing tips, the device guarantees the most remarkable clean – up to 2X as effective as string floss for improving gum health around implants with the Plaque Seeker™ tip.[xi]
The 360° tip rotation and guided routine with timed pacers establish an easy-to-use oral care regimen for all implant patients. The countertop water flosser offers professional oral care from the comfort of home. Its large-capacity reservoir provides thorough daily irrigation without interruption – guaranteeing longevity in patients’ implants as the #1 water flosser brand recommended by dental professionals.[xii]
Conclusion
Implant dentistry is transforming the lives of patients continuously. With a greater population of such patients, the measures of maintaining the longevity of treatment are increasingly important. Precautionary measures are the most effective when genuinely assimilated into everyday routines. Interdental plaque control is vital, but with traditional flossing methods underachieving both clinically and compliance-wise, alternatives must be recommended.
With easy-to-use, effective methods being recommended, clinicians protect their patients’ investment, develop long-term outcomes, and ensure that the implants remain healthy.
For more information on WaterpikTM water flosser products visit www.waterpik.co.uk. WaterpikTM products are available from Amazon, Costco UK, Argos, Boots and Tesco online and in stores across the UK and Ireland.
Recommend by brand
Author:
 Anne Symons is a Dental Hygienist currently working in a Specialist Periodontal/implant practice and also a busy NHS surgery. She has previously worked in a Max Fax unit, and also taught Oral Health care to staff in Nursing and Residential homes.
Anne Symons is a Dental Hygienist currently working in a Specialist Periodontal/implant practice and also a busy NHS surgery. She has previously worked in a Max Fax unit, and also taught Oral Health care to staff in Nursing and Residential homes.
[i] Heitz-Mayfield, L. Peri-implant mucositis and peri-implantitis: key features and differences. Br Dent J 236, 791–794 (2024). https://doi.org/10.1038/s41415-024-7402-z
[ii]Simon, F., Szabó, G., Orsós, M., Mijiritsky, E., & Németh, O. (2024). The Effectiveness of Individualized Oral Hygiene Education in Preventing Dental Diseases: A Clinical Study. Journal of Clinical Medicine, 13(18), 5481. https://doi.org/10.3390/jcm13185481.
[iii] Perussolo J, Donos N. Maintenance of peri-implant health in general dental practice. Br Dent J. 2024 May;236(10):781-789. doi: 10.1038/s41415-024-7406-8. Epub 2024 May 24. PMID: 38789755; PMCID: PMC11126374.
[iv] Saleh, Muhammad & Galli, Matthew & Siqueira, Rafael & Vera Rodriguez, Maria & Wang, Hom-Lay & Ravidà, Andrea. (2022). The Prosthetic-Biologic Connection and Its Influence on Peri-implant Health: An Overview of the Current Evidence. The International journal of oral & maxillofacial implants. 37. 690-699. 10.11607/jomi.9523.
[v] Soulami, Sara & Slot, Dagmar & van der Weijden, Fridus. (2022). Implant‐abutment emergence angle and profile in relation to peri‐implantitis: A systematic review. Clinical and Experimental Dental Research. 8. 10.1002/cre2.594.
[vi] Adult Oral Health Survey 2021: Health-related behaviours (no date) GOV.UK. Available at: https://www.gov.uk/government/statistics/adult-oral-health-survey-2021/adult-oral-health-survey-2021-health-related-behaviours (Accessed: 30 September 2025).
[vii] Thevissen E, De Bruyn H, Koole S. The provision of oral hygiene instructions and patient motivation in a dental care system without dental hygienists. Int J Dent Hyg. 2017 Nov;15(4):261-268. doi: 10.1111/idh.12211. Epub 2016 Mar 1. PMID: 26932773.
[viii] Healy, S.R. and Erdman, K.A. (2019) Strategies to maintain complex implant restorations, Dimensions of Dental Hygiene. Available at: https://dimensionsofdentalhygiene.com/article/strategies-to-maintain-complex-implant-restorations (Accessed: 26 September 2025).
[ix] Gandi, Gargi & Masanam, Bhoomika & Nair, Ananya & Semani, Nidhi & Chopra, Aditi & Venkitachalam, Ramanarayanan. (2025). Efficacy of oral irrigators compared to other interdental aids for managing peri-implant diseases: a systematic review. BDJ Open. 11. 10.1038/s41405-025-00301-3.
[x] AlMoharib, H.S., Alqasem, A., Almusfer, G. et al. The effectiveness of water jet flossing and interdental flossing for oral hygiene in orthodontic patients with fixed appliances: a randomized clinical trial. BMC Oral Health 24, 498 (2024). https://doi.org/10.1186/s12903-024-04166-0
[xi] Mahajani MJ, Kalla M, Sonkesriya S, Mehra P, Laddha R, Akade G. Comparison of the Impact of Two Interdental Cleaning Devices on the Reduction of Bleeding Around Implants. J Pharm Bioallied Sci. 2024 Feb;16(Suppl 1):S192-S195. doi: 10.4103/jpbs.jpbs_453_23. Epub 2024 Feb 29. PMID: 38595601; PMCID: PMC11001108.
[xii] Based on 2025 independent survey of Dental Professionals; among those who recommended branded water flossers.




