
The word depression often evokes connotations of the emotional struggles associated – persistent sadness, fatigue, hopelessness, and so many more. But one of the less understood effects of depression is the intense impact it has on physical health, specifically oral health.[i] This connection is often overlooked but affects the overall welfare of so many people worldwide.
Depression alters everyday habits detrimentally, and oral hygiene is one of the first routines to suffer the consequences. Due to the diminishment in energy and motivation that comes with depression, it has a profound impact on oral health due to neglected oral hygiene procedures.[ii] For so many people living with depression, simple tasks like brushing or flossing can feel overwhelming and are avoided. This can lead to countless oral health issues, some even lifelong.
The cycle between depression and oral health is vicious; the consequences of poor oral hygiene can cause greater depressive symptoms, and in turn, lead to even poorer maintenance of oral care, continuously.[iii]
The bidirectional breakdown
When individuals neglect their oral health due to circumstances beyond their control, an array of problems begin, including an increased risk of periodontal disease, avoidance of necessary dental care, dental caries, and even tooth loss.[iv] The scientific evidence supports the spiralling effect between depression and oral health, proving that the level of oral hygiene is insufficient in those suffering.[v] As mentioned, this relationship is a bidirectional continuum.
As such, improving and maintaining good oral health offers better prospects for the long-term stability of mental health. With oral care being better prioritised, the risk of long-term implications is reduced and the likelihood of invasive, expensive treatment being required is minimised. Fewer necessary dental treatments doesn’t only mean better economic outcomes, but with the avoided financial stress, mental health can improve too.[vi]
Various obstacles in motivation
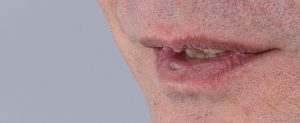
Medication also plays a significant role as antidepressant-induced xerostomia is a major risk associated with it.[vii] Saliva is crucial in maintaining oral health, rinsing excess food particles, preventing bacteria growth, and neutralising the pH balance.[viii] Many antidepressants note dry mouth as a common side effect due to a decreased production of saliva. The likelihood of suffering from halitosis when experiencing depression is greatly increased too, stemming from the dry mouth and the lack of interdental hygiene.[ix] Furthermore, these issues leave individuals that take antidepressants at a much higher risk of cavities, gingivitis, and other long-term effects, many of which they will not have the necessary mental enthusiasm to address.[x]
The physical symptoms of depression and their interference with self-care are often under-acknowledged. Fatigue, muscle aches, and increased sleep disturbances can eventually build to make tedious tasks like tooth brushing feel physically exhausting.[xi] Something that once felt a twice-daily task now feels like a tiresome obligation. Furthermore, the psychological toll surrounding depression includes feelings of extreme low self-worth. Suffering individuals may believe that they don’t deserve access to health care and the passive self-harm is warranted – avoiding essential measures and sustaining the depressive pit they’re stuck in. Moreover, some individuals often actively avoid dental appointments all together due to extended feelings of anxiety, shame, and fear of judgement.[xii]
Small steps outweigh stagnancy
When the emotional tax makes self-care seem impossible, energy and mindsets are low, and routine has faltered, brushing can seem too great of an effort, with all oral care falling on the priority list. Due to this, establishing a feasible oral health routine which can be attained through accessible, easy-going actions can make a world of difference and help to break the vicious cycle.[xiii]
 One product that offers effective daily protection to a daily oral care routine is the Perio Plus Balance mouthrinse from Curaprox. Featuring an innovative pleasant tasting alcohol-free formula, it contains effective anti-bacterial agents Chlorhexidine (0.05%) and Citrox as well as sodium fluoride to provide additional protection against caries too. It can also help provide relief from complications like dry mouth and halitosis, offering a professionally endorsed oral rinse from the comfort of patients’ homes. Perio Plus Balance can also help support daily oral care routines for those with impaired motor skills, with the PVP/VA ingredient providing a long-lasting protective film over the teeth and gingiva, effectively helping to reduce common oral health problems to leave users feeling fresher and cleaner.
One product that offers effective daily protection to a daily oral care routine is the Perio Plus Balance mouthrinse from Curaprox. Featuring an innovative pleasant tasting alcohol-free formula, it contains effective anti-bacterial agents Chlorhexidine (0.05%) and Citrox as well as sodium fluoride to provide additional protection against caries too. It can also help provide relief from complications like dry mouth and halitosis, offering a professionally endorsed oral rinse from the comfort of patients’ homes. Perio Plus Balance can also help support daily oral care routines for those with impaired motor skills, with the PVP/VA ingredient providing a long-lasting protective film over the teeth and gingiva, effectively helping to reduce common oral health problems to leave users feeling fresher and cleaner.
Seizing personal control of oral health
When people feel personally empowered in taking small steps towards reclaiming their health, the effects can transfer to mental health too. Improving oral health can ease discomforts and enhance confidence, eventually building to improved mental health and wellbeing. Breaking vicious cycles and unfavourable bidirectionality allows for positive progress and steps in the right direction towards good health. Recovery is never about perfection – establishing a flawless oral health routine is not always feasible – but supporting manageable consistency always leads to positive outcomes.

To arrange a Practice Educational Meeting with your Curaden Development Manager please email us on sales@curaden.co.uk
For more information, please visit www.curaprox.co.uk and www.curaden.co.uk
Author: Andrew Turner

[i] Mirza I, Day R, Phelan M, Wulff-Cochrane V. Oral health of psychiatric in-patients: A point prevalence survey of an inner-city hospital. Psychiatric Bulletin. 2001;25(4):143-145. doi:10.1192/pb.25.4.143
[ii] Heaton LJ, Santoro M, Tiwari T, Preston R, Schroeder K, Randall CL, et al. Mental Health, Socioeconomic Position, and Oral Health: A Path Analysis. Prev Chronic Dis 2024;21:240097. DOI: http://dx.doi.org/10.5888/pcd21.240097
[iii] Z K, Siluvai S, Kanakavelan K, et al. (December 23, 2024) Mental and Oral Health: A Dual Frontier in Healthcare Integration and Prevention. Cureus 16(12): e76264. doi:10.7759/cureus.76264
[iv] Skośkiewicz-Malinowska, K., Malicka, B., Ziętek, M., & Kaczmarek, U. (2018). Oral health condition and occurrence of depression in the elderly. Medicine, 97(41), e12490. https://doi.org/10.1097/MD.0000000000012490
[v] Stepović, M., Stajić, D., Rajković, Z., Maričić, M., & Sekulić, M. (2020). Barriers Affecting the Oral Health of People Diagnosed with Depression: A Systematic Review. Zdravstveno varstvo, 59(4), 273–280. https://doi.org/10.2478/sjph-2020-0034
[vi] Asiri, A., Nazir, M.A., Alsharief, M. et al. Effect of psychological distress on oral health: a cross-sectional study. BMC Oral Health 24, 1508 (2024). https://doi.org/10.1186/s12903-024-05319-x
[vii] Skośkiewicz-Malinowska, K., Malicka, B., Ziętek, M., & Kaczmarek, U. (2018). Oral health condition and occurrence of depression in the elderly. Medicine, 97(41), e12490. https://doi.org/10.1097/MD.0000000000012490
[viii] Nath, S., Zilm, P., Jamieson, L. et al. The influence of diet, saliva, and dental history on the oral microbiome in healthy, caries-free Australian adults. Sci Rep 15, 18755 (2025). https://doi.org/10.1038/s41598-025-03455-0
[ix] Vali, A., Roohafza, H., Keshteli, A. H., Afghari, P., Javad Shirani, M., Afshar, H., Savabi, O., & Adibi, P. (2015). Relationship between subjective halitosis and psychological factors. International dental journal, 65(3), 120–126. https://doi.org/10.1111/idj.12153
[x] Taccardi, D., Chiesa, A., Maiorani, C., Pardo, A., Lombardo, G., Scribante, A., Sabatini, S., & Butera, A. (2024). Periodontitis and Depressive Disorders: The Effects of Antidepressant Drugs on the Periodontium in Clinical and Preclinical Models: A Narrative Review. Journal of Clinical Medicine, 13(15), 4524. https://doi.org/10.3390/jcm13154524
[xi] Bair MJ, Robinson RL, Katon W, Kroenke K. Depression and Pain Comorbidity: A Literature Review. Arch Intern Med. 2003;163(20):2433–2445. doi:10.1001/archinte.163.20.2433
[xii] Patel, R., Gamboa, A. Prevalence of oral diseases and oral-health-related quality of life in people with severe mental illness undertaking community-based psychiatric care. Br Dent J 213, E16 (2012). https://doi.org/10.1038/sj.bdj.2012.989
[xiii] Z, K., Siluvai, S., Kanakavelan, K., Agnes, L., Kp, I., & G, K. (2024). Mental and Oral Health: A Dual Frontier in Healthcare Integration and Prevention. Cureus, 16(12), e76264. https://doi.org/10.7759/cureus.76264




